
Foundations of theranostics
Radioligand therapy (RLT) and radioligand imaging (RLI) offer a novel, theranostic approach to targeting and treating certain types of cancer.1 This section of the Novartis RLT Institute is designed to help health care professionals (HCPs) understand the basic scientific foundations of RLT. By focusing on the science, we aim to demystify radiation and safety concerns and build confidence in offering patients this approach to precision medicine in cancer.
Multidisciplinary teams
A successful RLT program typically requires communication, planning, and coordination among a multidisciplinary team (MDT) involving multiple specialties and individuals, with each member of the team helping to fulfill specific roles to streamline the process and deliver quality patient care.2,3
Individual practices and responsibilities for RLT may vary on the basis of institutional organization and available resources.3 All multidisciplinary teams can optimize RLT treatment by collaborating in key areas, such as4:
- Treatment eligibility: establishing a consensus on appropriate treatment eligibility and understanding the imaging, pathology, and clinical scenarios required for therapy
- Communication: communicating regularly, with the health care team connecting frequently through either an established meeting or routine communication, as established by the relationships
- Navigation systems: establishing navigation systems with a clinical coordinator who champions the process, arranges visits, and communicates with the patient, serving as a backbone for communication with support staff for both referring teams and additional support teams
- Accountability: enabling quality care with established principles and holding team members accountable
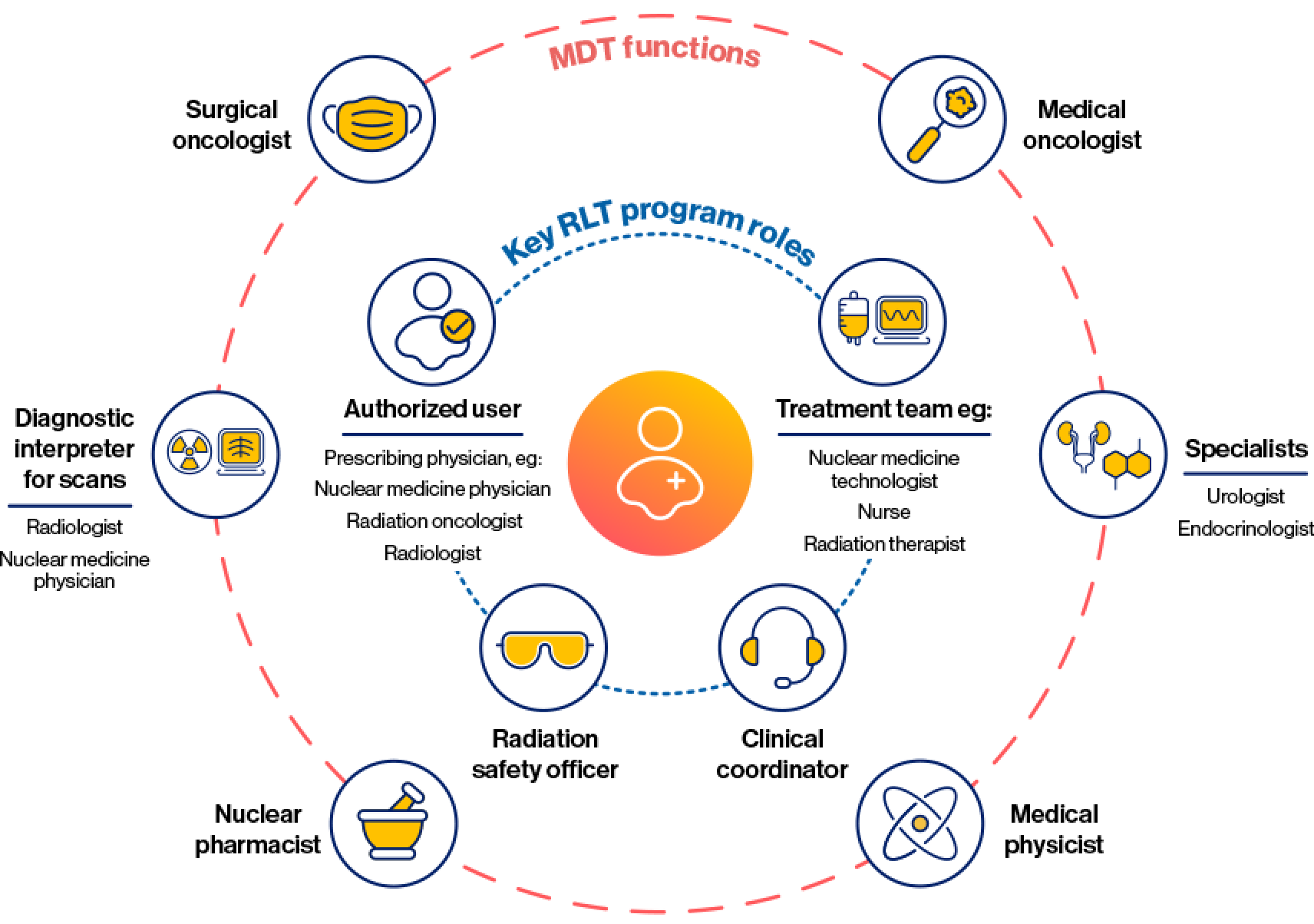
Key RLT program roles
Distinct from medical specialties, the following roles provide essential functions for operating a successful RLT program and may be fulfilled by various individuals, depending on the practice3:

AUs
Authorized users (AUs) are authorized to handle, use, and supervise the use of radioactive materials. They are the prescribing physician for RLT, typically a nuclear medicine physician, radiation oncologist, or radiologist.3
See more about AU responsibilities and getting certified
Radiation safety officer
The radiation safety officer (RSO) ensures safe handling and use of radioactive materials, implements the radiation safety program, provides safety training, and reports incidents. An AU may also be the RSO.3,4
See more about RSO responsibilities and getting certified
Treatment team
The treatment team sets up and manages the RLT infusion under the supervision of the AU. This may include appropriately trained nuclear medicine technologists, radiation therapists, and/or nurses.4

Clinical coordinator
Clinical coordinators navigate patients through authorization, scheduling, and visits, communicating with both patients and the MDT. This role may be fulfilled by a number of individuals, including nurse navigators, front desk staff, and nuclear medicine technologists.4


Expert insight
Consider appointing a “center champion” to lead the initiation, development, and implementation of the RLT program, unite the MDT, and take primary responsibility for the successful operation of the program.4
MDT functions
Several medical disciplines contribute to patient care with RLTs. These HCPs often include but are not limited to the following individuals3,4:

Nuclear medicine physician
Nuclear medicine physicians specialize in the use of radiopharmaceuticals to treat patients and in the diagnostic interpretation of imaging scans. As the designated AU, they may prescribe RLT for patients. They may also be involved in determining patient eligibility, ordering RLTs, administering concomitant medications, monitoring patients for adverse events, and managing side effects.2-4

Radiation oncologist
Radiation oncologists specialize in the use of ionizing radiation to treat patients with cancer. They may be a referring physician or, as the designated AU, they may prescribe RLT for patients. They may also be involved in determining patient eligibility, ordering RLTs, administering concomitant medications, monitoring patients for adverse events, and managing side effects.2,3,6

Nuclear medicine technologist
In accordance with the radiation safety protocols set by the RSO and informed by federal and local regulations, the technologist's responsibilities may include ordering RLTs from manufacturers, receiving, documenting, and inspecting doses upon arrival, preparing RLT doses, obtaining intravenous access, administering the RLT under AU supervision, monitoring patients during therapy, performing radiation surveys of the treatment areas, and, upon treatment conclusion, ensuring that the patient’s radiation level is below the threshold established by the RSO prior to discharge.2,3,7

Radiation therapist
In accordance with the radiation safety protocols set by the RSO and informed by federal and local regulations, a radiation therapist may be responsible for safe handling and delivery of RLT, monitoring patients for adverse events, performing radiation surveys of the treatment areas, and, upon treatment conclusion, ensuring that the patient’s radiation level is below the threshold established by the RSO prior to discharge.8

Nurse
In accordance with the radiation safety protocols set by the RSO and informed by federal and local regulations, nurses (ie, therapy room or cancer infusion room nurses) may be responsible for safe handling and delivery of RLT, obtaining intravenous access, administering concomitant medications, and monitoring patients for adverse events.2,3
Nurse navigators or other outpatient clinic nurses may focus on coordinating RLT activities including patient communication, scheduling, orientation, education, and postdischarge events.3

Medical oncologist
Medical oncologists may be involved in collaboration with the AU in the day-to-day care and co-management of cancer patients, including referring appropriate patients and monitoring patients during RLT treatment and posttreatment follow-up.2,3

Surgical oncologist
Surgical oncologists, especially in cancers involving surgical intervention, may be the partner physician referring patients for RLT, ensuring prevention of interference with other planned treatments, providing care coordination, helping to assess treatment tolerance and response to therapy, and managing toxicities.3

Medical physicist
Medical physicists (radiation oncology physicists and nuclear medicine physicists) are responsible for overseeing the accreditation and quality control programs for nuclear medicine imaging equipment. As qualified experts, their role includes designing and reviewing quality control programs, testing equipment used for imaging and therapy, and designing structural radiation shielding.3

Nuclear pharmacist
Nuclear pharmacists ensure the quality, safety, and efficacy of radiopharmaceuticals. They compound and/or prepare radioligand imaging agents and may prepare RLTs, if needed, before administration. As manufactured products typically do not require additional compounding and/or preparation, nuclear pharmacists can sometimes be off-site or outsourced.2,4

Radiologist
Radiologists may play a crucial role in partnering with oncologists in multidisciplinary cancer care teams, offering expertise in medical imaging for diagnosis, treatment planning, and monitoring of cancer patients. With appropriate certification and training, a radiologist may be an AU.3,9

Pathologist
Pathologists may assess tissue samples to confirm diagnosis and subsequent biopsies to optimize care.10-12

Urologist
For prostate cancer, urologists may play a key role in assessing patients for RLT. They provide expertise on the patient’s urological condition and determine if they are suitable candidates for RLT, typically in collaboration with nuclear medicine physicians and/or radiation oncologists to manage individualized treatment approaches for the patients.5,10,13

Endocrinologist
For hormone-related cancers such as gastroenteropancreatic neuroendocrine tumors (GEP-NETs), endocrinologists may play a key role in assessing patients for RLT. They may oversee the patient's RLT treatment plan, monitor hormone levels, and manage potential side effects related to the therapy.14-16

Other HCPs
Other HCPs may include but are not limited to psychologists, palliative care specialists, social workers, primary care providers, genetic counselors, physiologists/dieticians, and other tumor-specific specialists who refer the patient for RLT treatment.3,10,17
